When Grammy Award-winning singer LeAnn Rimes opened up about her lifelong battle with eczema, she revealed how the condition had affected her confidence and comfort for decades. “Having to constantly hide my skin became exhausting,” she shared in a candid interview. Her experience resonates with the estimated 31 million Americans living with this challenging skin condition, particularly among African American communities where prevalence rates run significantly higher.
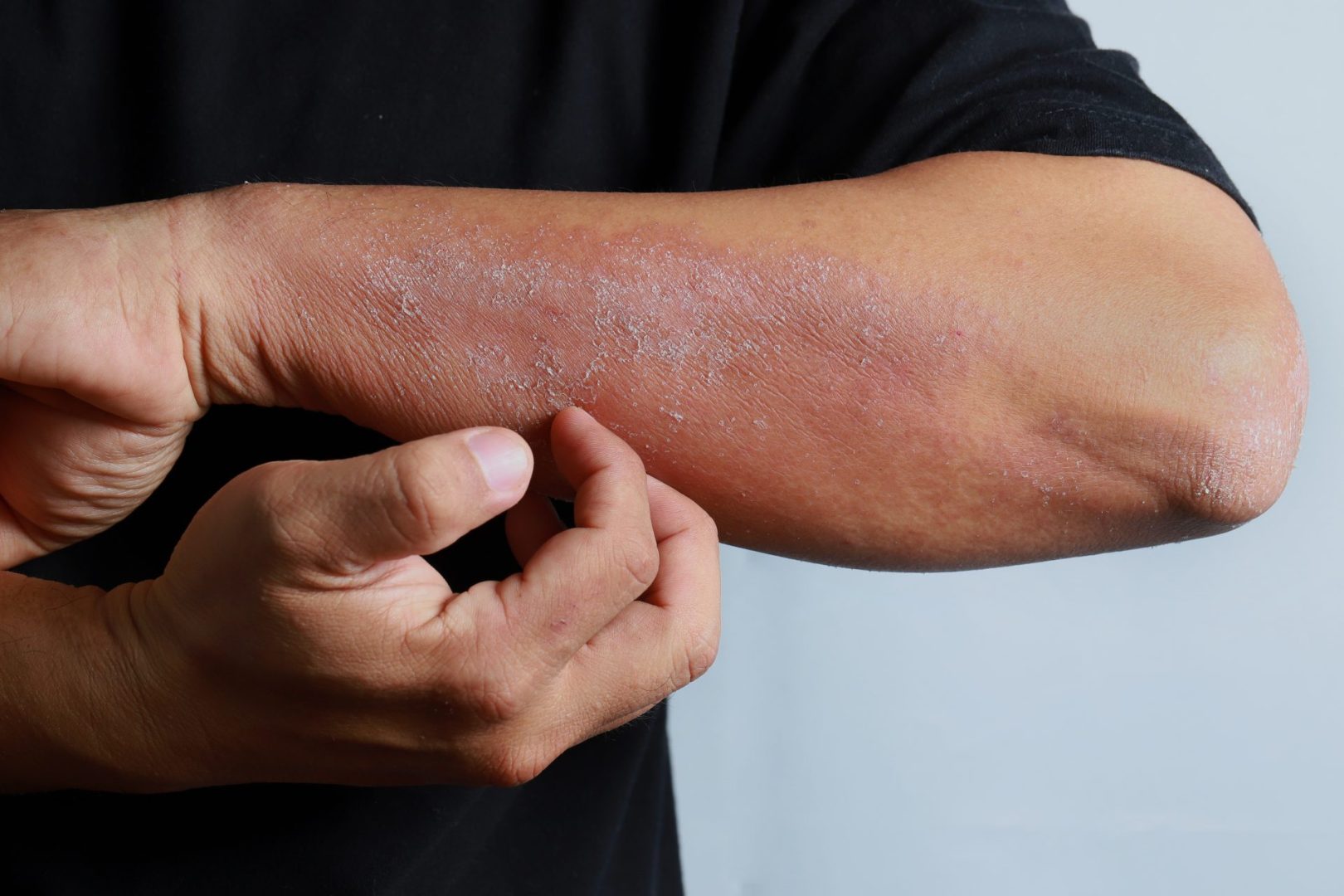
Atopic dermatitis, the most common form of eczema, creates a frustrating cycle of itching, scratching, and inflammation that can disrupt sleep, social activities, and overall quality of life. Yet many sufferers remain unaware of recent advances in understanding and treating this condition. The latest research reveals that effective management involves more than just topical creams, with a multi-faceted approach offering the best chance for long-term relief.
Why eczema happens and who gets it most
At its core, atopic dermatitis results from a compromised skin barrier combined with an overactive immune response. The skin’s protective barrier, which normally locks in moisture and blocks irritants, becomes damaged in eczema patients. This allows moisture to escape while permitting environmental triggers to penetrate the skin, setting off inflammatory reactions that create the characteristic red, itchy patches.
Genetic factors play a significant role in determining who develops this condition. Research has identified mutations in the filaggrin gene, which helps maintain skin barrier function, as a common factor among many patients. Those with a family history of eczema, asthma, or hay fever face higher risks of developing the condition themselves due to shared genetic susceptibilities across these allergic disorders.
Ethnicity appears to influence both prevalence and severity patterns. Studies show that African American children experience eczema at nearly twice the rate of their white peers, with symptoms often presenting as more severe and persistent. This disparity extends into adulthood, with darker skin tones frequently experiencing more intense inflammation and greater impacts on quality of life.
Environmental factors trigger flare-ups in those genetically predisposed to the condition. Common culprits include harsh soaps, synthetic fabrics, pet dander, pollen, and certain foods. Climate conditions also influence symptom severity, with cold, dry winter air and high humidity environments both capable of worsening symptoms for different individuals.
Stress levels correlate strongly with symptom intensity. During periods of high stress, the body releases inflammatory compounds that can trigger or intensify eczema flares. This creates a challenging cycle where the discomfort of eczema generates stress, which in turn worsens the condition.
The telltale signs that confirm atopic dermatitis
Intense itching represents the hallmark symptom of atopic dermatitis, often preceding visible skin changes. This relentless itch, described by many sufferers as “maddening,” frequently disrupts sleep and concentration. The medical term “pruritus” barely captures the intensity patients experience, with many reporting that the urge to scratch feels completely uncontrollable, especially at night.
Distinctive skin changes vary by individual but follow recognizable patterns. In lighter skin tones, affected areas typically appear as reddened patches with small bumps. On darker skin, these areas may appear darker brown, purple, or grayish, sometimes making diagnosis more challenging for practitioners unfamiliar with these presentation differences. The skin often develops a leathery, thickened texture from repeated scratching and inflammation, a condition dermatologists call “lichenification.”
Location patterns provide important diagnostic clues. Children typically develop symptoms on the face, scalp, and outer limbs, while adults most commonly experience flares on neck, inner elbows, behind knees, hands, and feet. These distribution patterns help distinguish atopic dermatitis from other skin conditions with similar appearances.
Symptom intensity fluctuates over time, with periods of relative calm punctuated by intense flare-ups. These flares can last days, weeks, or even months without proper intervention. Many patients report a worsening of symptoms during seasonal transitions, particularly in fall and winter when indoor heating systems reduce humidity levels.
Secondary complications frequently accompany severe cases. Repeated scratching damages the skin’s protective barrier, creating entry points for bacteria, viruses, and fungi. Staphylococcus aureus infections particularly plague eczema patients, recognizable by increased redness, weeping, crusting, and sometimes fever. These infections require prompt medical attention and often antibiotic treatment.
The breakthrough treatments dermatologists recommend first
Modern dermatology offers increasingly effective solutions for managing atopic dermatitis, with treatment approaches tailored to symptom severity and individual needs. The foundation begins with reliable barrier repair through intensive moisturization. Dermatologists recommend applying moisturizers within three minutes after bathing, when skin remains slightly damp, to trap maximum hydration.
Pharmaceutical options have expanded significantly in recent years. Topical corticosteroids remain the first-line treatment for active inflammation, available in varying potencies from mild over-the-counter hydrocortisone to prescription-strength formulations. These medications reduce itching, redness, and swelling, but require careful application following medical guidance to avoid potential side effects like skin thinning with prolonged use.
Non-steroidal alternatives provide options for sensitive areas or long-term management concerns. Topical calcineurin inhibitors like tacrolimus and pimecrolimus target immune system responses without the skin-thinning effects of steroids, making them suitable for delicate areas like eyelids and face. These medications work by blocking specific immune pathways involved in inflammation.
Biological treatments represent the newest frontier for severe cases. Dupixent (dupilumab), the first biologic approved for atopic dermatitis, targets specific immune proteins driving inflammation. Administered by injection every two weeks, this breakthrough treatment has provided life-changing relief for many with severe, treatment-resistant eczema. Clinical trials showed that 37% of patients achieved clear or almost clear skin after 16 weeks of treatment.
Phototherapy using narrowband ultraviolet B (UVB) light offers another effective option for widespread eczema. This controlled exposure to specific wavelengths of UV light reduces inflammation and itching by modulating immune responses in the skin. Treatment typically involves 2-3 weekly sessions for several months, with many patients experiencing significant improvement after 10-15 sessions.
Daily habits that prevent painful flare-ups
Beyond medical treatments, specific lifestyle modifications significantly impact symptom management. Bathing practices require special attention, with dermatologists recommending short, lukewarm showers or baths lasting less than 10 minutes. Hot water, though temporarily soothing, ultimately worsens symptoms by stripping natural oils. Gentle, fragrance-free cleansers should replace conventional soaps, which often contain irritating detergents and artificial fragrances.
Clothing choices directly affect skin comfort. Loose-fitting cotton garments allow skin to breathe while minimizing friction against sensitive areas. Synthetic fabrics like polyester and nylon often exacerbate symptoms by trapping heat and moisture. Washing new clothing before wearing removes manufacturing residues that might trigger reactions, while using fragrance-free, dye-free detergents reduces exposure to common irritants.
Home environment modifications can dramatically reduce symptom triggers. Maintaining indoor humidity between 45-55% with humidifiers counteracts the drying effects of heating and air conditioning systems. Regular dusting and vacuuming with HEPA filters reduces dust mite exposure, a common trigger for many patients. Removing carpet in favor of hard flooring further reduces allergen accumulation.
Temperature regulation helps prevent the itch-scratch cycle. Overheating commonly precedes intense itching episodes, making strategies to maintain cool skin temperatures essential. Lightweight, breathable bedding, moisture-wicking fabrics during exercise, and avoiding excessive bundling in winter can prevent the perspiration that often triggers flares.
Stress management techniques directly impact skin health through the mind-body connection. Regular practice of relaxation methods such as deep breathing, progressive muscle relaxation, or meditation can reduce stress-induced inflammatory responses. Some patients benefit from working with mental health professionals to develop personalized stress management strategies and address the psychological impact of living with a visible chronic condition.
The surprising diet connection researchers are studying
Emerging research suggests dietary factors may influence eczema severity for some individuals, though specific effects vary considerably between patients. Anti-inflammatory foods including fatty fish rich in omega-3 fatty acids, colorful fruits and vegetables high in antioxidants, and probiotic-containing fermented foods may help modulate immune responses and reduce inflammation in some patients.
Food sensitivity testing remains controversial among dermatologists. While some patients report dramatic improvement after eliminating specific foods, controlled studies show mixed results. Common trigger foods include dairy, eggs, nuts, soy, gluten, and certain fruits. Rather than eliminating multiple foods simultaneously, dermatologists typically recommend supervised elimination trials of one food category at a time, followed by careful reintroduction to identify specific triggers.
Gut health increasingly appears connected to skin health through what researchers call the “gut-skin axis.” Studies show that eczema patients often have altered gut microbiome compositions compared to those without the condition. Probiotic supplements containing specific bacterial strains have shown modest benefits in some clinical trials, particularly for children with moderate to severe symptoms.
Essential fatty acid balance may influence inflammation levels. Modern diets typically contain excessive omega-6 fatty acids (found in vegetable oils and processed foods) compared to omega-3 fatty acids (found in fatty fish, flaxseeds, and walnuts). This imbalance potentially promotes inflammatory responses. Increasing omega-3 intake while reducing processed food consumption may help reduce overall inflammation.
Hydration status directly affects skin barrier function. Adequate daily water intake helps maintain skin hydration from within, supporting the skin’s natural moisture balance. While drinking water alone cannot resolve eczema, insufficient hydration can worsen skin dryness and compromise barrier function.
Natural remedies with scientific backing
Several natural approaches have gained scientific support for symptom management, though they typically work best alongside conventional treatments rather than replacing them. Colloidal oatmeal baths, recognized by the FDA as a skin protectant, create a soothing, moisturizing layer that relieves itching and reduces inflammation. Adding one cup of colloidal oatmeal to lukewarm bathwater provides immediate comfort during flares.
Certain plant oils demonstrate beneficial properties for compromised skin barriers. Cold-pressed sunflower seed oil contains essential fatty acids that help repair skin barrier function. Virgin coconut oil exhibits both moisturizing and antimicrobial properties, potentially reducing Staphylococcus aureus colonization common in eczema patients. Always perform patch testing before applying new products to larger skin areas.
Cold therapy provides immediate itch relief through temperature-sensitive nerve pathways. Applying cold compresses for 5-10 minutes can interrupt the itch-scratch cycle during intense flares. Following cold therapy with moisturizer application maximizes benefits by sealing in hydration while the cooling effect temporarily reduces itching sensation.
Diluted bleach baths show efficacy for preventing infections in severe eczema. This approach, while sounding harsh, has solid research support. Adding ¼ to ½ cup of regular household bleach to a full bathtub of water (approximately 40 gallons) creates a solution similar to chlorinated pool water that reduces bacterial colonization on skin. These baths, limited to twice weekly for 5-10 minutes, should be followed by thorough rinsing and immediate moisturizing.
Evening primrose oil supplements, containing gamma-linolenic acid (GLA), have shown modest benefits in some studies. This essential fatty acid helps reduce inflammation through its effects on prostaglandin production. While not effective for everyone, some patients report improvement with regular supplementation, typically requiring several weeks before noticeable effects appear.
When to seek specialized medical care
Certain situations warrant prompt medical attention rather than continued self-management. Suspected skin infections require professional evaluation. Signs include increased pain, warmth, swelling, yellow crusting, honey-colored drainage, or sudden worsening of symptoms. These infections may require prescription antibiotic treatments to resolve properly.
Severe sleep disruption from nighttime itching deserves medical intervention. Chronic sleep deprivation impacts overall health, immune function, and quality of life. Dermatologists can recommend specialized evening treatment routines and medications specifically targeting nighttime symptoms to break this debilitating cycle.
Emotional distress resulting from visible skin symptoms affects many patients. Studies show increased rates of anxiety and depression among those with moderate to severe atopic dermatitis. Mental health impacts deserve attention, with dermatologists increasingly recognizing the importance of addressing psychological aspects alongside physical symptoms.
Treatment-resistant cases benefit from specialist evaluation. Dermatologists with expertise in atopic dermatitis can identify subtle diagnostic factors, recommend advanced treatment options, or detect underlying complications. These specialists often practice at academic medical centers or dedicated eczema clinics where comprehensive management approaches integrate multiple treatment modalities.
Extensive body surface involvement, typically defined as affecting more than 10% of total skin area, may require systemic treatment approaches rather than topical management alone. These widespread cases often indicate immune dysfunction requiring medications that address underlying inflammatory pathways rather than just surface symptoms.
Living well despite chronic symptoms
Successful long-term management extends beyond medical treatments to include practical coping strategies. Building a consistent skincare routine forms the foundation of effective management. Daily practices become protective rituals, with most dermatologists recommending simpler regimens focused on consistent moisturizing rather than complex multi-step approaches that may introduce additional irritants.
Environmental adaptations minimize exposure to common triggers. Home modifications like removing carpeting, using allergen-proof mattress covers, maintaining optimal humidity levels, and installing air purification systems reduce continuous exposure to irritants. These changes create a “safe zone” where skin can heal during vulnerable periods.
Patient education improves treatment adherence and outcomes. Understanding the chronic, relapsing nature of atopic dermatitis helps manage expectations and maintain motivation during difficult periods. Knowledge about specific triggers, early signs of flares, and appropriate treatment escalation empowers patients to intervene effectively before symptoms become severe.
Support networks provide both emotional sustenance and practical knowledge. Online communities connect patients facing similar challenges, while in-person support groups foster understanding relationships. These connections combat the isolation many experience, particularly during visible flare periods when social withdrawal becomes tempting.
Perspective shifts transform the experience of living with chronic skin symptoms. Rather than viewing eczema as an enemy to defeat, many long-term patients develop approaches that acknowledge the condition as a part of life requiring management rather than a battle requiring victory. This mindset reduces the emotional burden while maintaining committed self-care practices.
Most importantly, those living with atopic dermatitis should remember that treatment options continue expanding through ongoing research. The pipeline of new medications targeting specific immune pathways offers hope for even the most severely affected patients. By working closely with healthcare providers, staying informed about emerging options, and maintaining consistent self-care practices, most people with atopic dermatitis can achieve significant symptom control and maintain good quality of life despite this challenging condition.