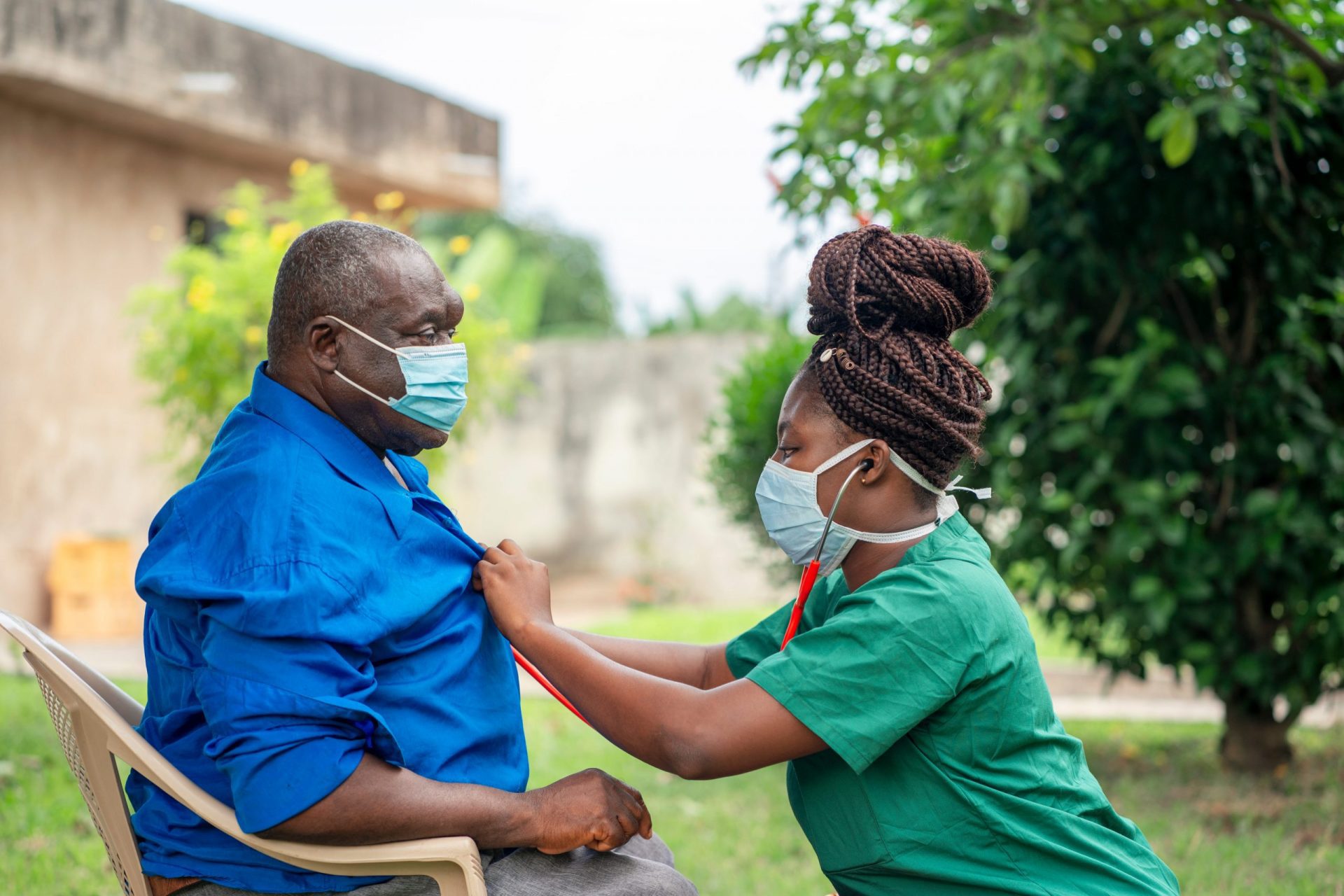
Heart disease silently stalks Black communities across America, claiming lives prematurely and devastating families without warning. As the second leading cause of death among Black men—only surpassed by cancer—this health crisis demands immediate attention yet often develops without symptoms until reaching dangerous stages.
Health statistics tell a sobering story: Black men die from heart disease at significantly higher rates than other demographic groups, with many deaths occurring during what should be the prime years of life. This disparity represents not just a medical concern but a complex social issue requiring comprehensive solutions.
Medical experts emphasize that while the statistics appear daunting, heart disease remains largely preventable through lifestyle modifications, regular health monitoring, and community support systems. Understanding the specific risk factors affecting Black men provides crucial knowledge for protecting heart health and potentially saving lives.
The following seven facts highlight essential information about cardiovascular disease and offer practical guidance for prevention, early detection, and treatment. This knowledge represents a critical first step toward addressing this preventable health crisis and creating healthier futures for Black men and their communities.
The silent progression that makes heart disease especially dangerous
The first essential fact involves understanding how cardiovascular disease typically develops without obvious warning signs. Unlike conditions that produce clear symptoms, heart disease often progresses silently for years before manifesting as a life-threatening event.
This silent progression makes regular health screenings absolutely critical for Black men. Blood pressure checks, cholesterol monitoring, and heart rhythm assessments can detect problems before they become emergencies. Many men discover their cardiovascular disease only after experiencing a heart attack or stroke, when preventive opportunities have already been missed.
Medical research shows that nearly 50 percent of Black men have some form of cardiovascular disease by age 60, yet many remain unaware of their condition. This knowledge gap highlights the importance of proactive health monitoring rather than waiting for symptoms to appear.
The danger extends beyond the individual, as undetected heart conditions can lead to sudden death, leaving families without fathers, brothers, sons, and partners. This devastating impact ripples through communities, creating multigenerational trauma and economic hardship for families losing primary providers.
Understanding this silent progression motivates regular medical check-ups and creates awareness about subtle warning signs that might otherwise be dismissed. Symptoms like unusual fatigue, periodic shortness of breath, or occasional chest discomfort warrant immediate medical attention rather than a “wait and see” approach.
The blood pressure connection that dramatically increases risk
The second critical fact centers on hypertension’s role as the single most significant risk factor for heart disease among Black men. Often called the “silent killer,” high blood pressure damages blood vessels and heart tissue while producing few noticeable symptoms.
Black men develop hypertension earlier in life and experience more severe forms compared to other demographic groups. By age 55, approximately 75 percent of Black men have high blood pressure, compared to about 55 percent of white men. This earlier onset provides more time for blood vessel damage to accumulate, increasing heart attack and stroke risk.
Medical experts attribute this disparity to multiple factors, including genetic predisposition, dietary patterns, stress exposure, and environmental influences. The higher prevalence of salt sensitivity among Black individuals means that sodium consumption has a more pronounced effect on blood pressure compared to other populations.
Regular blood pressure monitoring represents the most effective defense against this risk factor. Home monitoring devices provide valuable information between medical visits, allowing for earlier intervention when readings begin trending upward. Many community health centers and pharmacies offer free blood pressure checks, removing financial barriers to this essential screening.
Treatment approaches increasingly recognize the need for culturally tailored interventions that address the specific patterns of hypertension in Black men. These approaches combine medication when necessary with lifestyle modifications that consider cultural dietary preferences and social contexts.
The stress connection that few doctors discuss
The third essential fact involves chronic stress’s profound impact on cardiovascular health, particularly for Black men navigating systemic inequities and daily microaggressions. Stress triggers physiological responses that directly damage the cardiovascular system when experienced persistently over time.
When the body remains in a chronic stress state, stress hormones like cortisol and adrenaline remain elevated, causing blood pressure increases, inflammation throughout the body, and changes to heart rhythm. These physical changes accelerate the development of atherosclerosis—the narrowing of arteries that precedes most heart attacks.
Research indicates that experiences of racial discrimination create chronic stress that manifests physically, contributing to earlier onset of hypertension and heart disease. This “weathering” effect accelerates biological aging of the cardiovascular system, creating health disparities that persist even when controlling for traditional risk factors.
Addressing this stress connection requires both individual stress management strategies and broader social changes. For individuals, practices like mindfulness meditation, regular physical activity, and adequate sleep help reduce stress hormones and their cardiovascular effects. Community connections and strong social support networks also buffer against stress’s negative impacts.
Health providers increasingly recognize the importance of screening for psychological stress during medical visits with Black male patients. This holistic approach acknowledges that effective heart disease prevention must address both physical and psychological aspects of health.
The nutrition barriers undermining heart health
The fourth critical fact examines how food environment disparities create significant obstacles to heart-healthy eating for many Black men. Neighborhood food access dramatically shapes dietary choices, with many predominantly Black communities lacking affordable sources of fresh produce and heart-healthy proteins.
Food deserts—neighborhoods without grocery stores offering fresh, affordable foods—characterize many urban and rural communities where Black families live. In these areas, convenience stores and fast-food restaurants become default food sources, offering primarily processed options high in sodium, unhealthy fats, and refined carbohydrates.
The economic reality of food costs further complicates heart-healthy eating. When feeding a family on a limited budget, calorie-dense processed foods often provide more affordable sustenance than fresh produce and lean proteins. This economic pressure creates difficult choices between financial stability and optimal nutrition.
Culturally traditional foods present both challenges and opportunities for heart health. While some traditional soul food preparations involve cooking methods and ingredients that can raise cardiovascular risk, these cultural food traditions can be modified to retain cultural significance while improving nutritional profiles.
Addressing these nutrition barriers requires both individual strategies and systemic changes. For individuals, batch cooking heart-healthy meals, buying frozen vegetables when fresh options are unavailable, and learning modified cooking techniques for traditional dishes represent practical approaches. At the community level, farmers’ markets accepting SNAP benefits, community gardens, and cooking education programs help create more equitable food environments.
The medical system barriers preventing proper care
The fifth essential fact addresses how healthcare system barriers prevent many Black men from receiving timely cardiovascular care. These barriers create situations where heart disease progresses untreated despite being highly manageable with proper medical intervention.
Lack of health insurance represents the most obvious barrier, with Black men more likely to work in jobs without employer-provided coverage. Without insurance, preventive care becomes financially inaccessible, and many men avoid seeking medical attention until emergencies occur.
Even with insurance, many Black communities lack sufficient healthcare providers, creating “medical deserts” where residents must travel significant distances for care. This geographic barrier becomes particularly problematic for preventive services and chronic disease management that require regular visits.
Past negative experiences with healthcare providers contribute to delayed care-seeking for many Black men. Experiences of dismissal, inadequate pain management, or perceived disrespect create justified hesitation about engaging with the medical system, even when symptoms warrant attention.
Work scheduling conflicts present practical barriers when medical appointments require taking unpaid time off. The choice between lost wages and preventive health services becomes particularly difficult for those in hourly wage positions without sick leave benefits.
Addressing these barriers requires both policy changes and community-based solutions. Expanded insurance coverage, increased funding for community health centers, and workforce diversity initiatives can help create more accessible healthcare. Community-based health outreach programs that bring screening services directly to neighborhoods and workplaces help bypass transportation and scheduling barriers.
The exercise roadblocks hindering prevention
The sixth critical fact examines how environmental and social factors create significant obstacles to regular physical activity for many Black men. While exercise provides powerful protection against heart disease, neighborhood conditions often determine whether regular activity feels accessible and safe.
Many predominantly Black neighborhoods lack safe spaces for outdoor activity due to concerns about crime, traffic dangers, or poorly maintained infrastructure. Without safe walking paths, parks, or recreation facilities, incorporating regular movement into daily life becomes significantly more challenging.
Gym memberships and fitness equipment represent financial investments inaccessible to many families prioritizing basic necessities. This economic barrier limits access to structured exercise environments, particularly during extreme weather when outdoor activity becomes impractical.
Long work hours and commute times create time barriers to regular exercise, particularly for those working multiple jobs or facing long public transportation journeys. When basic daily responsibilities consume available time, finding additional hours for structured physical activity presents a significant challenge.
Addressing these exercise barriers requires creative approaches at both individual and community levels. For individuals, home-based exercise routines requiring minimal equipment, incorporating movement into daily activities, and finding accountability partners help overcome some obstacles. At the community level, church-based fitness programs, school facility sharing during non-school hours, and workplace wellness initiatives create more accessible opportunities for physical activity.
The prevention strategies that work best for Black men
The seventh essential fact focuses on evidence-based prevention approaches specifically effective for Black men. While heart disease statistics appear daunting, research shows that targeted prevention strategies can dramatically reduce risk when consistently applied.
Regular health screenings represent the foundation of effective prevention, with blood pressure checks, cholesterol testing, and diabetes screening revealing problems before they cause permanent damage. Research indicates that community-based screening programs in trusted locations like barbershops and churches reach men who might otherwise avoid medical settings.
The DASH dietary approach (Dietary Approaches to Stop Hypertension) shows particular effectiveness for Black men in managing blood pressure—a primary heart disease risk factor. This eating pattern emphasizes fruits, vegetables, lean proteins, and whole grains while limiting sodium, sugar, and unhealthy fats, providing flexible guidelines adaptable to various food preferences.
Smoking cessation provides immediate cardiovascular benefits, with heart attack risk beginning to decrease within days of quitting. Culturally tailored cessation programs addressing the specific marketing targeted at Black communities show greater success than generic approaches.
Weight management focused on modest, sustainable changes rather than dramatic short-term weight loss creates lasting cardiovascular benefits. Programs emphasizing gradual lifestyle modifications rather than restrictive dieting show better long-term adherence and outcomes.
Peer support groups specifically for Black men create environments where health concerns can be discussed openly without judgment. These groups combine accountability, information sharing, and emotional support, addressing both practical and psychological aspects of heart health.
Medical advocates who help navigate healthcare systems improve outcomes by ensuring appropriate care and follow-through. Whether family members, community health workers, or patient advocates, these supporters help overcome communication barriers and ensure thorough care.
By focusing on these evidence-based approaches, Black men can significantly reduce their heart disease risk despite systemic challenges. When combined with broader policy changes addressing healthcare access and environmental factors, these strategies create paths toward cardiovascular health equity.
Understanding these seven critical facts about heart disease provides essential knowledge for protecting cardiovascular health. While the statistics remain concerning, increasing awareness, implementing prevention strategies, and addressing systemic barriers can help reduce heart disease’s devastating impact on Black men and their communities.
With continued focus on both individual prevention and systemic change, the future holds promise for reducing this health disparity and ensuring more Black men live long, heart-healthy lives with their families and communities.